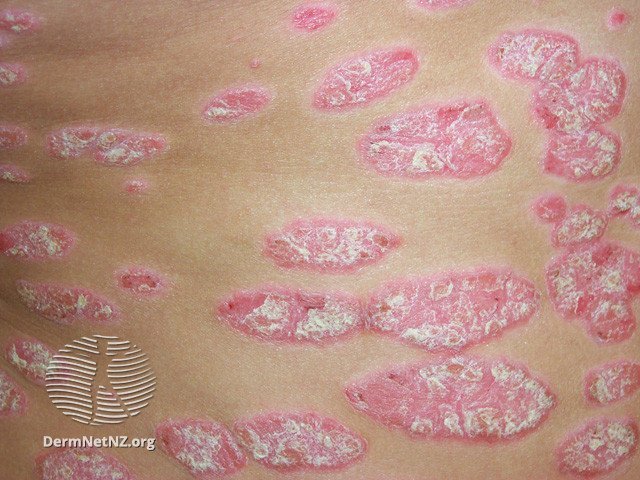
Psoriatic Arthritis
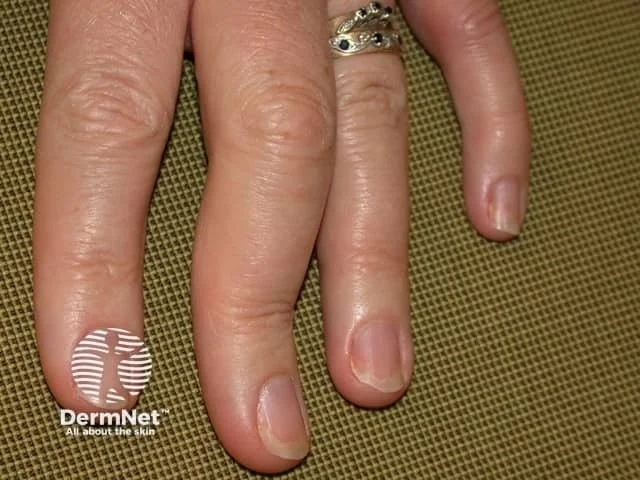
Longstanding psoriatic arthritis has damaged the joint, which is now showing a swan neck deformity.
Credit: DermNet NZ
What is Psoriatic Arthritis?
Psoriatic arthritis is a chronic inflammatory condition related to the immune system that affects the joints and the places where tendons and ligaments attach to bone. It most often occurs in people who also have psoriasis, although joint symptoms can sometimes appear before the skin disease is recognized. Roughly 1 in 3 people living with psoriasis also have psoriatic arthritis.
How does Psoriatic Arthritis relate to psoriasis?
Psoriatic arthritis and psoriasis are part of the same broader inflammatory disease process. The severity of psoriasis on the skin does not necessarily predict how severe the arthritis may be. Some patients have relatively limited skin disease but more significant joint involvement. Because of that overlap, dermatologists often help identify possible psoriatic arthritis and work with rheumatologists when joint symptoms are present.
What are possible signs and symptoms of Psoriatic Arthritis?
Common symptoms can include joint pain, swelling, stiffness, morning stiffness after rest, sausage-like swelling of fingers or toes, heel or foot pain related to enthesitis, nail changes such as pitting or lifting, and sometimes back pain. Psoriatic arthritis can affect one or many joints and, if not treated appropriately, can lead to ongoing inflammation and joint damage over time.
How is Psoriatic Arthritis diagnosed?
Psoriatic arthritis is usually diagnosed clinically rather than through one single definitive test. Evaluation may include a history, physical exam, review of skin and nail findings, bloodwork to help rule out other causes of joint symptoms, and imaging such as X-rays, ultrasound, or MRI when appropriate. It is typically best diagnosed and treated by a rheumatologist, and early diagnosis and treatment may help reduce the risk of permanent joint damage.
How is Psoriatic Arthritis treated?
Treatment depends on which joints or tendons are involved, whether the spine is affected, whether dactylitis or enthesitis is present, how much psoriasis is on the skin, symptom severity, prior treatment response, other medical issues, and the patient’s goals. Psoriatic arthritis is typically managed or co-managed by a rheumatologist (except in mild cases), and dermatologists often work with rheumatologists to choose treatments that can improve both psoriasis and arthritis symptoms.
Common treatment options include:
NSAIDs such as ibuprofen or naproxen for milder pain and stiffness
Corticosteroid injections into an affected joint when appropriate
Conventional disease-modifying medications such as methotrexate, sulfasalazine, or leflunomide
Oral targeted medications such as apremilast (Otezla), tofacitinib (Xeljanz/Xeljanz XR), or upadacitinib (Rinvoq)
Common biologic options currently used for psoriatic arthritis include:
TNF inhibitors such as adalimumab (Humira and biosimilars), etanercept (Enbrel), infliximab (Remicade and biosimilars), golimumab (Simponi, Simponi Aria), and certolizumab pegol (Cimzia)
IL-17 inhibitors such as secukinumab (Cosentyx), ixekizumab (Taltz), and bimekizumab-bkzx (Bimzelx)
IL-23 inhibitors such as guselkumab (Tremfya) and risankizumab-rzaa (Skyrizi)
IL-12/23 inhibitors such as ustekinumab (Stelara)
T-cell costimulation modulators such as abatacept (Orencia)
Biologic options have become increasingly targeted, and current treatments may focus on pathways such as TNF, IL-17, IL-23, or IL-12/23. In psoriatic arthritis, TNF inhibitors remain a very common treatment choice and are still often used as a first biologic option, especially for active joint disease. In practice, the best choice depends on the pattern of arthritis, the amount of skin and nail psoriasis, prior treatment response, other medical issues, dosing preferences, insurance coverage, and whether the main treatment goal is better control of joints, skin, or both.
Additional considerations
Patients with psoriasis should let their healthcare provider know about joint pain, prolonged morning stiffness, swollen fingers or toes, heel pain, or nail changes, since these can be clues to psoriatic arthritis. Regular follow-up is important, and exercise and general health maintenance also matter as part of long-term management.
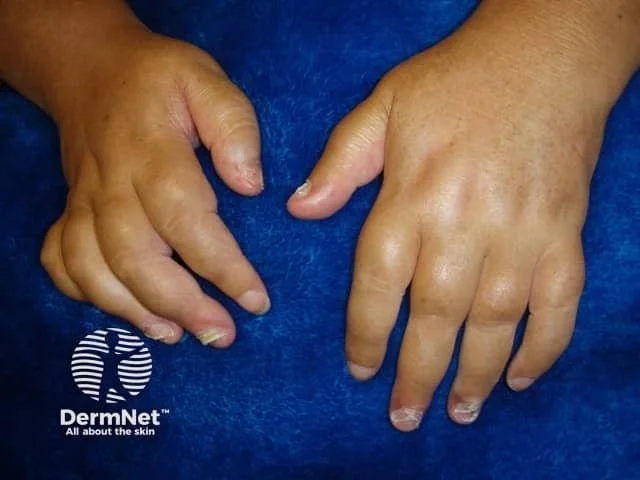
This is an example of psoriatic arthritis causing dactylitis (swelling of the fingers) and nail changes.
Credit: DermNet NZ
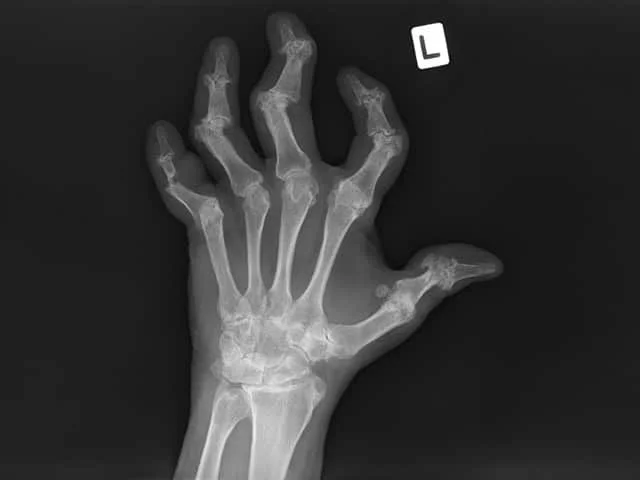
An example of Xray findings of mutilating joints in psoriatic arthritis, which can also occur in rheumatoid arthritis.
Credit: DermNet NZ
