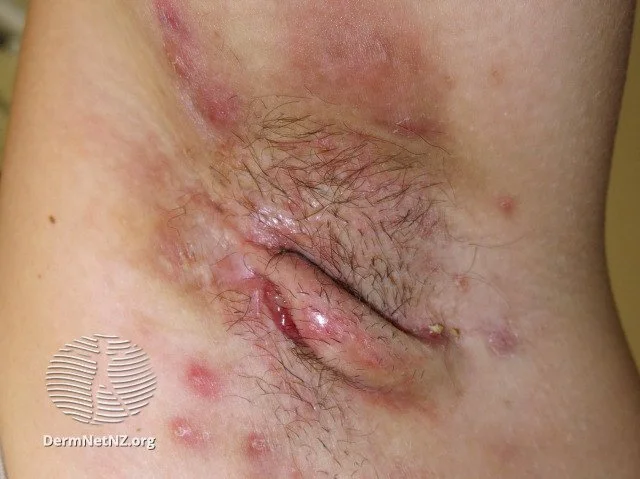
Hidradenitis Suppurativa
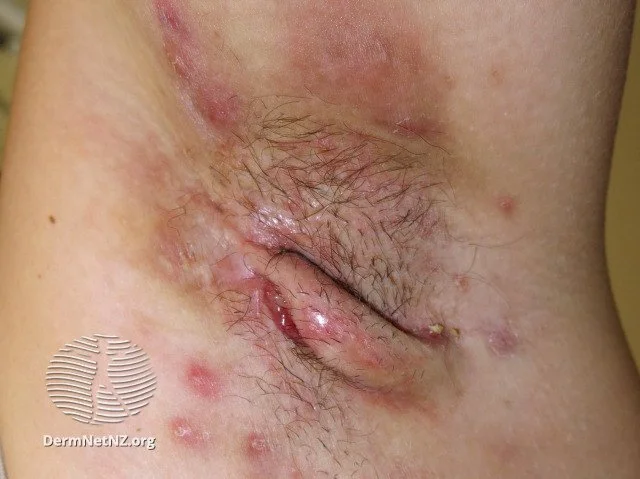
An example of hidradenitis suppurativa, which looks like boils, pimples, and scar-tissue tracts in the skin folds.
Credit: DermNet NZ
What is hidradenitis suppurativa?
Hidradenitis suppurativa, often shortened to HS, is a chronic inflammatory skin disease that causes painful bumps, nodules, abscesses, and draining areas in places where skin rubs together. Common sites include the underarms, groin, buttocks, inner thighs, and under the breasts.
HS is not simply a hygiene problem, and it is not just a series of ordinary boils. It is a long-term inflammatory condition that can scar over time and can have a major effect on pain, daily life, and confidence.
What causes hidradenitis suppurativa?
HS develops through a combination of follicular blockage, inflammation, genetics, and immune-system activity. It often begins after puberty and may flare on and off over time.
Known triggers or risk factors for HS encompass:
Hormonal Factors: Predominantly affecting women
Obesity: A significant contributing factor
Family History: Having relatives with HS increases risk
Smoking: Raises susceptibility
Clothing and Friction: Tight garments and chafing from skin folds
Shaving: Particularly in the affected areas
Autoimmune Disorders: Like inflammatory bowel disease
Certain Medications
Climatic Factors: Hot and humid weather can exacerbate symptoms
What are the symptoms of hidradenitis suppurativa?
Symptoms can include:
Painful lumps under the skin
Recurrent boils or abscess-like lesions
Drainage from inflamed areas
Tunnels under the skin, also called sinus tracts
Scarring and dark marks after flares
Tenderness, soreness, and limitation of movement in affected areas
HS can range from occasional isolated nodules to widespread, recurrent disease with scarring.
How is hidradenitis suppurativa treated?
Effective management of HS entails prevention, self-care, and lifestyle modifications, but medical intervention is often imperative. Potential treatments include:
Medications:
Antibiotics (oral forms like rifampicin/clindamycin, dapsone and topical clindamycin)
Hormonal treatments (birth control pills, spironolactone, finasteride)
Steroids (both injectable and oral forms for acute flare-ups)
Diabetes drug, Metformin
Acne medication, Isotretinoin
Immune-regulating drugs (methotrexate, cyclosporine, azathioprine)
Biologic treatments like adalimumab (Humira), infliximab (Remicade), secukinumab (Cosentyx), bimekizumab (Bimzelx) and JAK inhibitors
Surgical Options:
Draining of acute abscesses
Curettage and de-roofing of nodules, abscesses and sinuses
Laser ablation of nodules, abscesses and sinuses (typically not covered by insurance)
Surgical excision for persistent nodules
How do I prevent hidradenitis suppurativa flares?
Medication might be necessary for flare prevention, but individuals can also:
Adopt a healthy weight
Embrace an anti-inflammatory, plant-based diet low in sugars, grains, and dairy
Cease smoking
Choose loose clothing
Use fragrance-free antiperspirants daily
Maintain hygiene through antiseptic washes or bleach baths
Warm baths to soothe affected areas
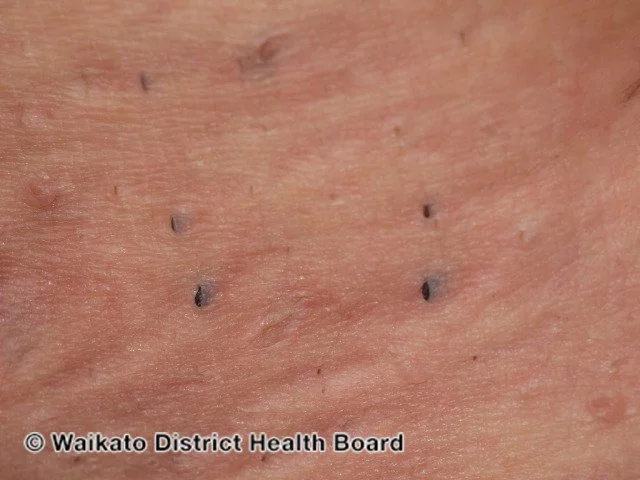
HS can cause comedones (clogged pores) in the affected areas - this is very characteristic.
Credit: DermNet NZ
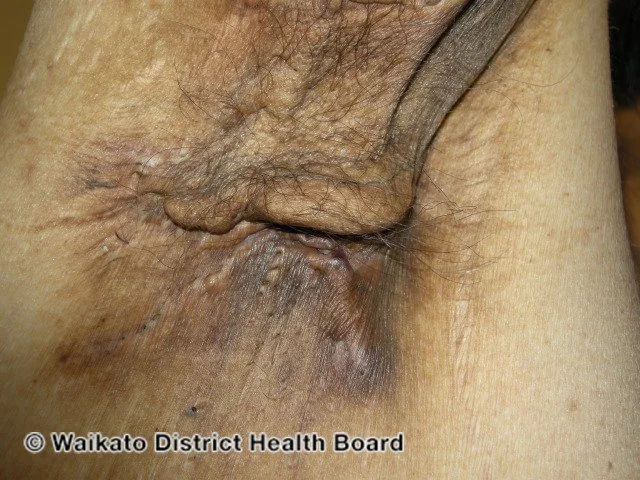
The scarring in hidradenitis suppurativa can be severe.
Credit: DermNet NZ
