Psoriasis: Causes, Symptoms and Treatment

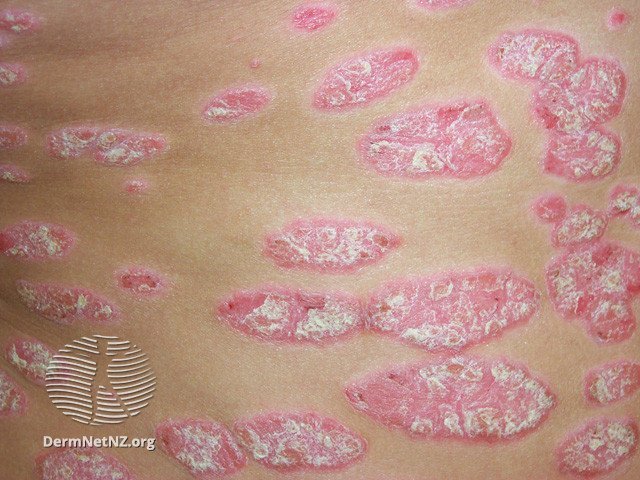
Plaque psoriasis, which demonstrates well-demarcated, red plaques with a classic silvery scale.
Credit: DermNet NZ
What is psoriasis?
Psoriasis is a chronic inflammatory skin disease that causes thick, scaly, inflamed plaques on the skin. It is driven by an overactive immune response that speeds up skin-cell turnover.
Plaque psoriasis is the most common form, but psoriasis can also affect the scalp, nails, skin folds, palms and soles, and in some cases large areas of the body. Some patients with psoriasis also develop psoriatic arthritis.
What causes psoriasis?
Psoriasis develops from a combination of immune-system activity, genetics, and environmental triggers. The skin cells turn over much faster than normal, leading to buildup of scale and inflammation.
Common triggers can include:
Obesity
Smoking
Excessive alcohol consumption
Illness or infections
Skin injuries, including cuts, burns, or tattoos
Significant life stressors
Reaction to certain medications, including lithium, beta-blockers, antimalarials, and NSAIDs
Abrupt cessation of steroid medications like prednisone
What are the symptoms of psoriasis?
Psoriasis manifests in diverse ways depending on its subtype. It typically appears as symmetrically distributed red, raised patches with clear borders, topped with a silvery-white scale. The affected areas can range from mildly to severely itchy, leading to potential skin thickening. Frequently affected regions include the scalp, elbows, and knees. The various subtypes of psoriasis exhibit specific symptoms:
Plaque Psoriasis: Predominantly appearing on the scalp, elbows, knees, and lower back, this is the most prevalent form and can sometimes be treatment-resistant.
Guttate Psoriasis: Identified by numerous small plaques, often following a streptococcal infection. Typically, it resolves within a few months.
Inverse Psoriasis: Occurs in body folds and genital regions, presenting as smooth, well-defined red patches.
Sebopsoriasis: Displays characteristics of both psoriasis and seborrheic dermatitis.
Palmoplantar Psoriasis: Specifically targets the palms and soles, leading to skin thickening and fissures.
Nail Psoriasis: Affects nails, causing discoloration, pitting, and separation of the nail bed.
Psoriatic Arthritis: Chronic inflammatory joint condition often associated with skin and nail psoriasis.
Generalized Pustular Psoriasis: A rare but potentially serious form of psoriasis that can cause sudden episodes of widespread red skin covered with many sterile pustules.
Erythrodermic Psoriasis: A rare, severe form, leading to a widespread peeling red rash. It may follow another type of psoriasis, often seen post steroid withdrawal, and is considered a medical emergency.
How is psoriasis treated?
Treatment depends on the type of psoriasis, the body areas involved, severity, symptoms, and the patient’s goals.
Common treatment options include:
Steroid-free topical options such as tapinarof (VTAMA) and roflumilast (Zoryve)
Oral medications such as apremilast (Otezla) or deucravacitinib (Sotyktu)
Common biologic options currently used for plaque psoriasis include:
IL-17 inhibitors such as secukinumab (Cosentyx), ixekizumab (Taltz), brodalumab (Siliq), and bimekizumab-bkzx (Bimzelx)
IL-23 inhibitors such as guselkumab (Tremfya), risankizumab-rzaa (Skyrizi), and tildrakizumab-asmn (Ilumya).
IL-12/23 inhibitors such as ustekinumab (Stelara)
TNF inhibitors (historically more common, although phasing out) such as adalimumab (Humira and biosimilars), etanercept (Enbrel), infliximab (Remicade and biosimilars), and certolizumab pegol (Cimzia)
Biologic options have become increasingly targeted, and current treatments may focus on pathways such as TNF, IL-17, IL-23, or IL-12/23. In practice, the best choice depends on skin severity, body areas involved, prior treatment response, other medical issues, dosing preferences, insurance coverage, and whether the patient also has psoriatic arthritis.
How can I help reduce psoriasis flares?
Helpful measures can include:
Using medications consistently as directed
Using moisturizers
Minimizing skin injury and picking
Reviewing possible medication triggers with your doctor
Managing related symptoms such as joint pain with appropriate medical evaluation
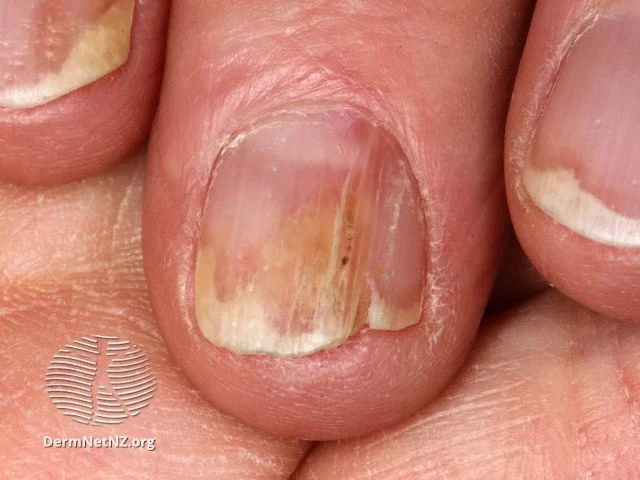
Nail psoriasis, which shows distal onycholysis (lifting of the nail plate), and oil spots (yellow spots where the psoriasis is in the nail bed).
Credit: DermNet NZ
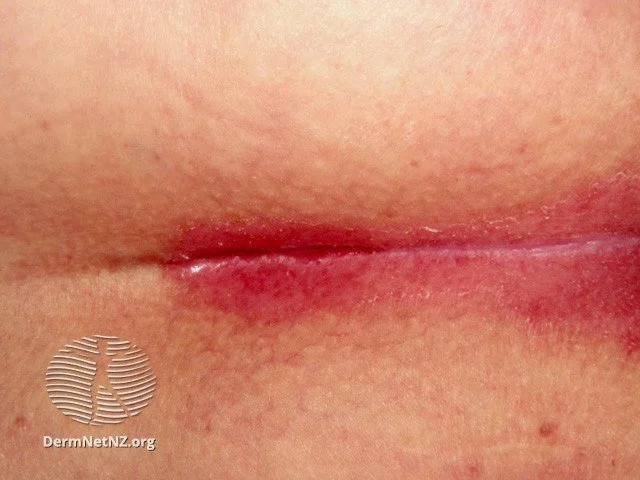
An example of inverse psoriasis, which manifests as red, smooth patches in body folds such as the gluteal crease or underneath the breasts.
Credit: DermNet NZ
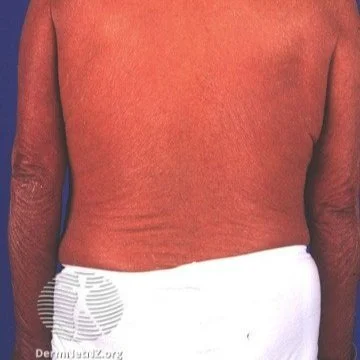
An example of erythrodermic psoriasis, which shows up as a sunburn-like rash on the whole body or almost the whole body.
Credit: DermNet NZ
